Get Help Today 24/7

When someone who has been drinking heavily suddenly stops, the brain can become dangerously overstimulated. That surge in activity can lead to shaking, confusion, and in some cases, seizures. Carbamazepine (Tegretol) is a medication sometimes used during drug and alcohol detox to help stabilize brain activity and lower seizure risk during this critical period.
3 Key Points
Table of Contents
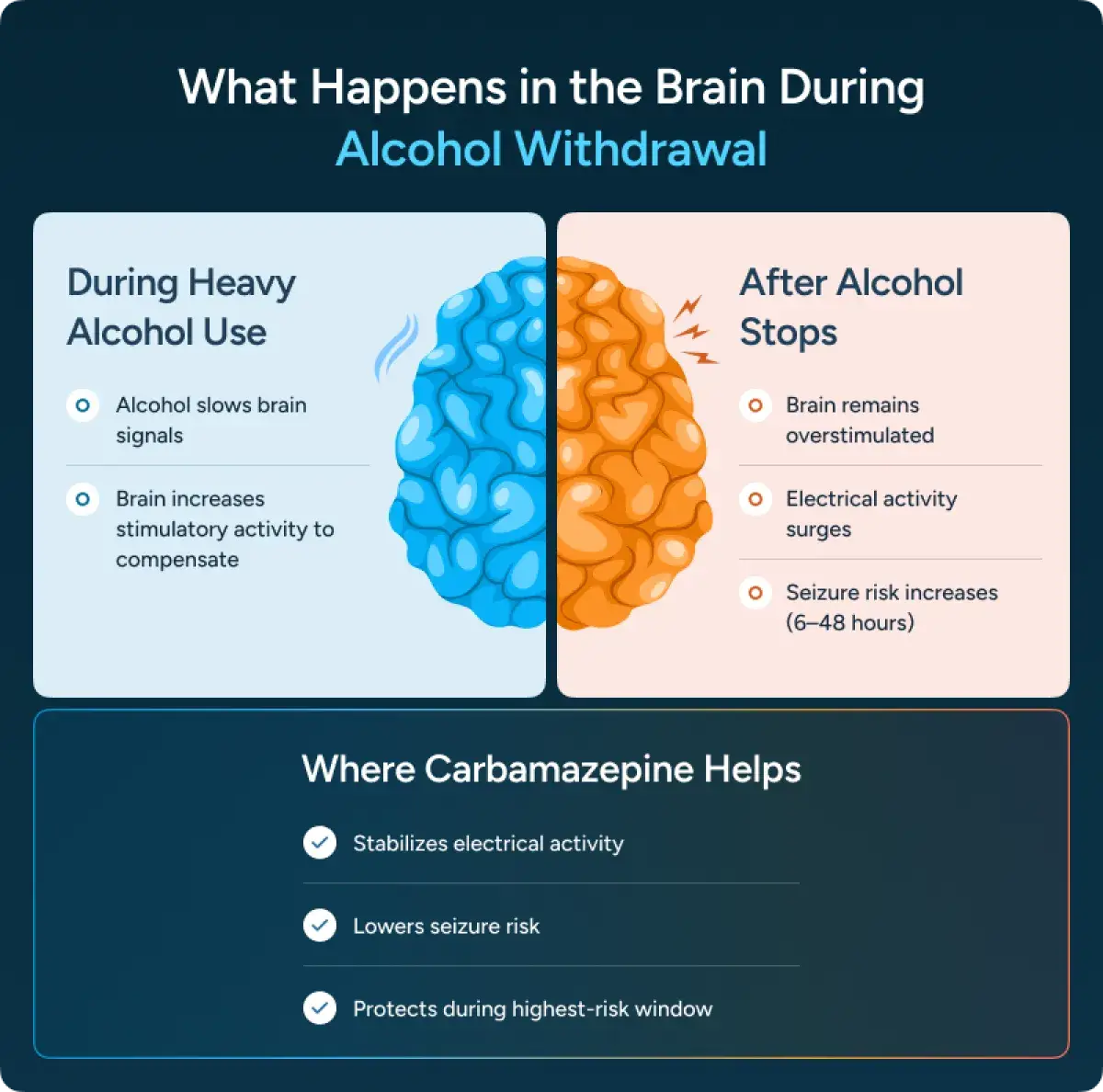
If someone has been drinking heavily for weeks, months, or years, their brain has adjusted to alcohol being present. Alcohol slows down brain activity. Over time, the brain tries to compensate by increasing its excitatory, or stimulating, signals. This keeps a person functioning while alcohol is in their system.
When alcohol suddenly stops, that balance is disrupted.
Instead of slowing signals, the brain can become overstimulated. This puts intense strain on the nervous system and can lead to:
Alcohol withdrawal seizures most commonly occur within 6 to 48 hours after the last drink. They can occur without warning, even in someone who has never had a seizure before.
This is why alcohol detox can become dangerous without a medically supervised detox setting.
Carbamazepine (brand name Tegretol) is an anticonvulsant medication. That means it is designed to reduce abnormal electrical activity in the brain.
During alcohol withdrawal, the brain can fire too rapidly. Think of it as a surge of electrical overactivity. Carbamazepine helps stabilize those signals, lowering the risk of seizures.
In mild to moderate alcohol withdrawal, it may help reduce:
It does not completely eliminate withdrawal symptoms. It also does not treat cravings for alcohol. Its role is primarily protective, helping the brain handle the stress of alcohol leaving the body.
In some cases, carbamazepine may be used instead of benzodiazepines, especially if there are concerns about sedation, misuse risk, or certain medical conditions.
The safest approach often involves a structured medical detox program based on drinking history, symptom severity, and overall medical health.
No. Carbamazepine is not considered addictive. It does not create a sedative “high” and is not associated with cravings the way benzodiazepines or opioids can be.
It is still a prescription medication that affects brain activity, so it must be used under medical supervision. In alcohol detox, it is typically used short term to reduce seizure risk while the body stabilizes.
Carbamazepine is not used in every case of alcohol withdrawal. The decision depends on how much someone has been drinking, their overall health, and their risk of serious complications.
Alcohol withdrawal can range from uncomfortable to life-threatening. Mild symptoms may include shakiness and anxiety. Severe withdrawal can involve seizures or delirium tremens (DTs), a dangerous condition marked by confusion, agitation, and unstable blood pressure or heart rate.
Medication plans are based on that risk level.
Carbamazepine is most often considered in mild to moderate cases within an alcohol detox program.
This may include:
During this stage, the brain is overstimulated but may not yet be in the highest danger category. Carbamazepine can help stabilize electrical activity in the brain and lower seizure risk while the body adjusts to the absence of alcohol.
It does not erase withdrawal symptoms. Its role is protective, helping reduce neurological strain during a vulnerable period.
Benzodiazepines are commonly used in alcohol detox, especially in moderate to severe cases. However, they are not ideal for every person.
Carbamazepine may be considered when:
Because carbamazepine works differently in the brain, it may offer an alternative in carefully selected situations.
Carbamazepine is not typically used alone in severe alcohol withdrawal or in cases with high seizure risk.
If someone has:
A more intensive detox protocol, often followed by residential treatment programs, is usually required.
Alcohol withdrawal can escalate quickly. Symptoms that seem manageable at first can become dangerous within hours. Medication decisions must match the severity of withdrawal and the person’s medical history.
The first 24 to 72 hours after the last drink carry the highest seizure risk. Close monitoring during this window provides the greatest protection.
No. Carbamazepine is not a benzodiazepine.
Benzodiazepines, such as diazepam (Valium) and lorazepam (Ativan), increase calming signals in the brain. They are commonly used during alcohol detox and are considered the first-line treatment for severe withdrawal because they quickly reduce seizure risk and nervous system overactivity.
Carbamazepine works differently. It stabilizes electrical activity inside brain cells rather than directly increasing calming chemicals. That difference matters.
Carbamazepine:
However, carbamazepine is not typically used alone in severe alcohol withdrawal or in cases with a high risk of delirium tremens (DTs), a life-threatening condition involving confusion, agitation, and unstable heart rate or blood pressure.
The safest medication approach depends on drinking history, past withdrawal symptoms, and overall medical health. A proper medical evaluation determines which option provides the most protection.
Carbamazepine can help lower seizure risk and reduce neurological overstimulation during alcohol withdrawal. For people with mild to moderate symptoms, this may help stabilize the detox process.
However, it is not a cure for alcohol withdrawal.
It does not:
Alcohol withdrawal is unpredictable. If withdrawal symptoms escalate, additional medications or a higher level of care may be required. Medication plans must adjust in real time based on symptoms and risk level.
Carbamazepine can be an important tool during alcohol withdrawal, but it is still a medication that affects the brain, blood chemistry, and liver. Because alcohol withdrawal already places strain on the body, any medication used during detox needs careful monitoring.
Understanding what is common versus what is serious can help you know what to expect.
Most people tolerate carbamazepine reasonably well, especially when dosing is adjusted carefully. The most common side effects include:
These effects often improve as the body adjusts. However, during alcohol withdrawal, symptoms can overlap. Shakiness, nausea, and fatigue may come from withdrawal itself rather than the medication.
That overlap is one reason medical supervision matters. It allows providers to tell the difference and adjust treatment if needed.
Carbamazepine is processed through the liver. If someone has been drinking heavily, the liver may already be inflamed or stressed. For that reason, blood work is often checked before or during treatment. Monitoring liver enzymes helps ensure the medication is not adding additional strain.
Carbamazepine can also lower sodium levels in the blood in some cases. Sodium plays a role in nerve and muscle function. When levels drop too low, a person may experience confusion, weakness, worsening headaches, or in rare cases, seizures. These changes are uncommon, but they are serious enough to require monitoring.
Although uncommon, carbamazepine has been associated with severe skin reactions. A spreading rash, blistering, or peeling skin requires immediate medical attention.
It can also affect bone marrow in rare cases, which may impact blood cell production. This is why ongoing monitoring is part of safe use.
Carbamazepine interacts with several other medications, including certain antidepressants, antipsychotics, blood thinners, and seizure medications. A full medical review is necessary before starting it.
Carbamazepine is not appropriate for everyone. It may not be recommended if there is:
Detox planning should always take into account overall health, drinking history, and withdrawal risk level.
Alcohol withdrawal is unpredictable. Medication choice, dosing, and monitoring must match the severity of symptoms and the person’s medical background. If new confusion, worsening tremors, severe vomiting, rash, or sudden changes in behavior occur, emergency medical care is necessary.
Detox is safest in a medical detoxification center where symptoms can be observed in real time and treated immediately if they escalate.
This is a common and important question. Carbamazepine does not make alcohol detox safe to attempt alone. Seizures can happen suddenly. Blood pressure can spike quickly. Dehydration and confusion can escalate fast.
Even when carbamazepine is prescribed, medical supervision is critical because:
If someone has a history of heavy daily drinking, past withdrawal seizures, or symptoms like hallucinations or severe shaking, detoxing at home can be extremely risky.
Alcohol withdrawal is unpredictable. The safest approach is a medical detox setting where symptoms can be monitored and treated immediately if they escalate.
Alcohol detox is not something you have to handle by yourself. Medical detox provides supervision, symptom support, and a plan that can adjust as your body responds. Whether a benzodiazepine or a non-benzodiazepine alcohol detox approach is used, the goal is the same: keeping you safe and as comfortable as possible.
Help is available, and getting support during detox can make a difficult process safer and less overwhelming.
Get answers about your cost / coverage now.
Your information will be kept private
Let’s talk about what’s going on — no judgment. (We’ve been there before ourselves). No one will know you inquired and there is no commitment to call.
Need someone to talk to? We’re always here—day or night.
Ask questions, get guidance—no pressure, no obligation.
Your story stays with us. Confidential support, always.


Why Wait?
Get Answers Now
You’re here because you know you need help. Let’s talk through it together. There’s no commitment and it’s 100% confidential even to check your insurance.
100% Confidential


Why Wait?
Get Answers Now
You’re here because you know you need help. Let’s talk through it together. There’s no commitment and it’s 100% confidential even to check your insurance.
100% Confidential