Get Help Today 24/7

When withdrawal starts, body aches and headaches tend to show up fast. Muscles hurt. Sleep is rough. Everything feels tense and uncomfortable. Most people reach for what they already know, like ibuprofen, naproxen, or Tylenol, hoping it will take the edge off.
Sometimes that works. Sometimes it causes more problems.
Detox puts a lot of stress on the body. Dehydration, nausea, and changes in how the liver and kidneys are working can all affect how safe these medications really are. A dose that feels harmless on a normal day may not be as safe during withdrawal.
Knowing which pain relievers are okay to use, which ones need extra caution, and when it’s better to avoid them altogether can help you detox safely.
Table of Contents
Ibuprofen, naproxen, and acetaminophen all help with pain, but they work in different ways inside the body. That difference matters during drug and alcohol detox.
NSAIDs stands for non-steroidal anti-inflammatory drugs. This group includes:
NSAIDs help with pain by reducing inflammation. Inflammation is part of what causes soreness, swelling, and aching muscles during withdrawal. These medications can be helpful for body aches and headaches, especially when inflammation is involved.
The downside is that NSAIDs can irritate the stomach and affect blood flow to the kidneys. During detox, when dehydration and stomach upset are common, that can increase the risk of side effects.
Acetaminophen, also known as Tylenol, works differently.
Acetaminophen is processed mainly by the liver. That makes it easier on the stomach and kidneys, but harder on the liver, especially after heavy or long-term alcohol use.
So while these medications are often grouped together, they don’t stress the same organs. During withdrawal, choosing the wrong one or taking too much can add extra strain to a body that is already working hard to stabilize.
During withdrawal, the body is already under stress. Pain relievers that feel routine in everyday life can act very differently when hydration is low, organs are strained, and symptoms are changing hour by hour.
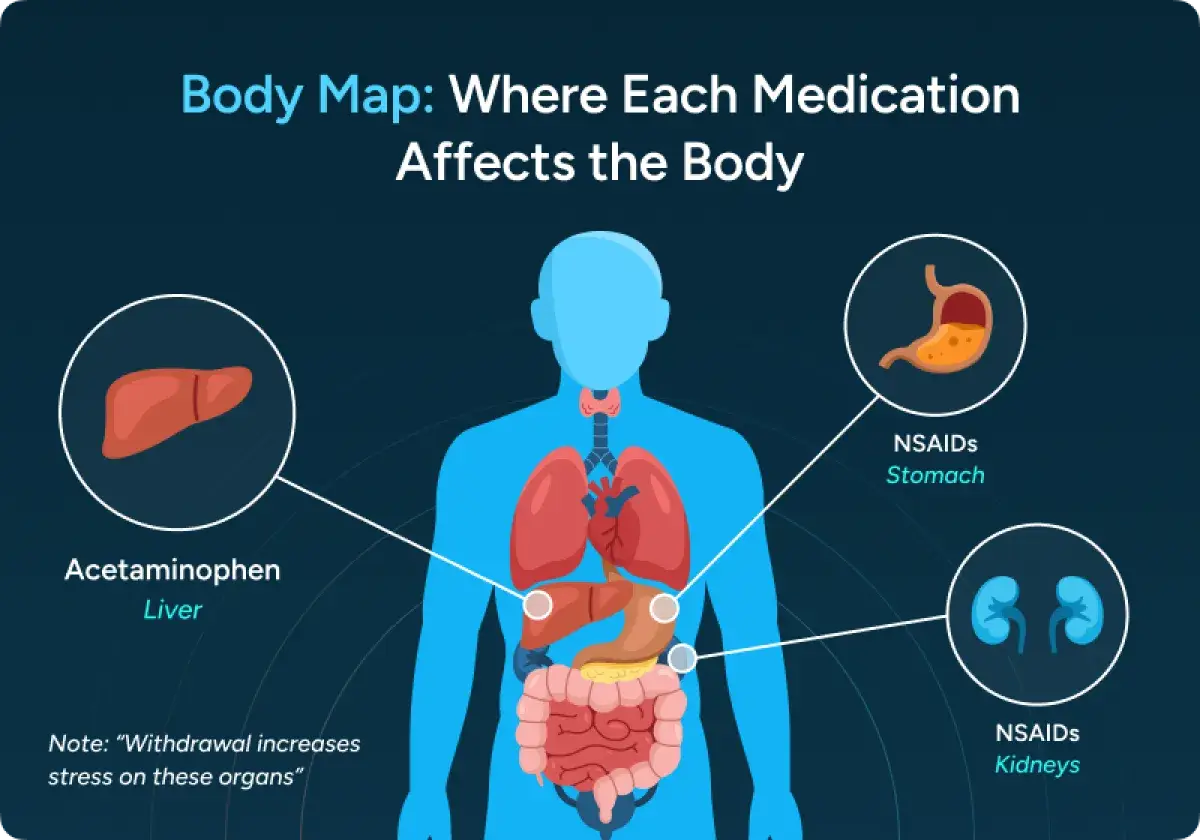
Vomiting, diarrhea, sweating, and poor fluid intake are common during withdrawal. Dehydration reduces blood flow to the kidneys and thickens the blood, which makes certain medications harder for the body to process safely.
NSAIDs are especially sensitive to this. When taken while dehydrated, they increase the risk of kidney injury and stomach irritation.
The liver plays a major role in detoxing both substances and medications. After heavy alcohol use, the liver is often inflamed or damaged, even if blood tests were normal in the past.
Acetaminophen is broken down in the liver. During withdrawal, especially alcohol withdrawal, repeated or higher doses can overwhelm the liver and increase the risk of injury.
Withdrawal can irritate the stomach lining and increase acid production. NSAIDs further thin the protective lining of the stomach, which raises the risk of:
This risk is higher for people detoxing from alcohol.
When pain feels intense, it’s tempting to take higher doses or doses more often. During withdrawal, this increases side effects without fixing the underlying cause of the pain.
Pain relievers can reduce discomfort, but they do not calm the nervous system, stop withdrawal symptoms, or prevent cravings.
NSAIDs are often used to help with body aches and headaches during withdrawal. In some cases, they can reduce discomfort. In others, they add risk. The difference depends on hydration, the substance involved, and overall health.
NSAIDs can be useful for:
They are sometimes used during opioid or stimulant withdrawal when fluid intake is stable and there are no kidney or stomach concerns. When taken at standard doses and for short periods, they may take the edge off physical discomfort.
NSAIDs are more likely to cause problems during detox when:
In these situations, NSAIDs increase the risk of kidney injury and stomach bleeding. Taking higher doses or using them repeatedly to push through withdrawal can make symptoms worse rather than better.
NSAIDs do not treat withdrawal itself. They do not reduce cravings or calm the nervous system. If pain feels severe or unmanageable, that is often a sign that medical detox support is needed.
While both NSAIDs and acetaminophen are common over-the-counter pain relievers, they affect the body very differently during detox.
Medication Type
Common Examples
What It Helps With
Main Risk During Detox
Extra Caution Needed When
NSAIDs
Acetaminophen
Ibuprofen (Advil, Motrin) Naproxen (Aleve)
Acetaminophen (Tylenol)
Muscle aches, joint pain, headaches related to inflammation
Headaches, mild to moderate body pain, fever
Kidney strain, stomach irritation, increased bleeding risk
Liver injury
Dehydration, vomiting or diarrhea, alcohol withdrawal, kidney disease
Alcohol detox, heavy or long-term drinking history, liver disease, using multiple products with acetaminophen
Medication Type
NSAIDs
Common Examples
Ibuprofen (Advil, Motrin) Naproxen (Aleve)
What It Helps With
Muscle aches, joint pain, headaches related to inflammation
Main Risk During Detox
Kidney strain, stomach irritation, increased bleeding risk
Extra Caution Needed When
Dehydration, vomiting or diarrhea, alcohol withdrawal, kidney disease
Medication Type
Acetaminophen
Common Examples
Acetaminophen (Tylenol)
What It Helps With
Headaches, mild to moderate body pain, fever
Main Risk During Detox
Liver injury
Extra Caution Needed When
Alcohol detox, heavy or long-term drinking history, liver disease, using multiple products with acetaminophen
Acetaminophen is often seen as the “gentler” option because it does not irritate the stomach the way NSAIDs can. During detox, that can be true in some situations. In others, it carries its own serious risks.
Acetaminophen may help reduce:
Because it does not thin the stomach lining or affect the kidneys in the same way NSAIDs do, it may be used cautiously when nausea or stomach irritation is already present.
Acetaminophen is processed almost entirely by the liver. Alcohol also stresses the liver, especially after long-term or heavy use.
During alcohol withdrawal, even “normal” doses of acetaminophen can increase the risk of liver injury. This risk goes up when:
Many cold, flu, and combination pain products already contain acetaminophen. It is easy to take more than intended without realizing it.
Acetaminophen can help with pain, but it does not protect the liver during withdrawal. If alcohol use is part of the picture, this medication should only be used with medical guidance.
Alcohol withdrawal places unique stress on the body. This changes how common pain relievers affect safety, even at doses that usually feel harmless.
Long-term or heavy drinking can inflame or damage the liver. During early alcohol detox, the liver is focused on stabilizing after alcohol is removed from the system.
Because acetaminophen is processed in the liver, repeated doses during this time increase the risk of liver injury. This risk exists even when doses stay within standard limits.
Alcohol irritates the stomach lining and affects how blood clots. NSAIDs further thin the stomach’s protective layer, which raises the risk of:
This combination makes NSAIDs a higher-risk option during alcohol withdrawal.
Sweating, vomiting, and poor fluid intake are common during alcohol detox. Dehydration increases the strain on the kidneys and worsens side effects from NSAIDs.
Alcohol withdrawal is unpredictable, which is why medically supervised alcohol detox is essential. Symptoms can escalate quickly, and medication choices need to account for liver health, hydration, and seizure risk.
Medical detox allows symptoms to be treated safely without increasing the risk of liver or stomach injury from over-the-counter pain relievers.
Opioid withdrawal is often described as feeling like a severe flu mixed with intense restlessness. Body aches, muscle pain, headaches, and cramping are common, especially in the first few days after opioids are stopped.
Pain relievers can play a small supportive role, but they have clear limits.
NSAIDs or acetaminophen may reduce:
When hydration is stable and doses stay within standard limits, these medications may take the edge off physical discomfort during opioid withdrawal.
Over-the-counter pain relievers do not:
They do not replace medications used specifically for opioid withdrawal, such as buprenorphine, clonidine, or lofexidine.
As opioid withdrawal intensifies, pain can feel overwhelming. Increasing the dose or taking pain relievers more often increases the risk of side effects without addressing the cause of the discomfort.
Severe or worsening pain during opioid withdrawal is often a sign that medically supervised withdrawal support is needed, not stronger over-the-counter medication.
Withdrawal from stimulants like cocaine or methamphetamine looks different from alcohol or opioid withdrawal. Physical pain is usually milder, but headaches, muscle soreness, and extreme fatigue are common.
How Pain Relievers May Be Used
NSAIDs or acetaminophen may help with:
When hydration is adequate and doses stay within standard limits, these medications are sometimes used short term.
What Matters More Than Pain Relievers
During stimulant withdrawal, discomfort is often driven by:
Pain relievers do not address these symptoms. Rest, hydration, nutritional support, and mental health care play a much larger role in stabilization.
If headaches or pain are severe, persistent, or worsening, medical evaluation is important to rule out dehydration, blood pressure issues, or other complications.

Over-the-counter pain relievers feel familiar, which makes it easy to underestimate their risks during detox. Many complications happen because of simple, well-intended mistakes.
Many cold, flu, and combination pain medications already contain acetaminophen. Taking more than one product at the same time can quickly push total daily doses higher than intended.
This is one of the most common causes of accidental liver injury during withdrawal.
Vomiting, diarrhea, and sweating increase fluid loss. Taking ibuprofen or naproxen while dehydrated raises the risk of kidney injury and stomach bleeding.
Drinking water alone does not always correct dehydration during withdrawal.
When pain feels intense, it’s tempting to take higher doses or doses more often. This increases side effects without treating the cause of withdrawal symptoms.
More medication does not equal better relief.
Pain relievers can reduce discomfort, but they do not stabilize withdrawal. Relying on them alone can delay proper care and increase medical risk.
Detox is safest when symptoms are monitored and medications are used appropriately.
Withdrawal affects more than just comfort. It changes how the body handles fluids, medications, and stress. That’s why managing pain during detox is not as simple as choosing the “right” over-the-counter medication.
With medically supervised detox:
This reduces the risk of complications like dehydration, liver injury, kidney strain, and internal bleeding.
Medical detox also allows symptoms to be addressed as they change. Withdrawal is not static, and medication needs often shift over the first several days.
Trying to manage severe withdrawal at home often leads to either under-treating symptoms or overusing medications that carry risk.
Some withdrawal symptoms should not be managed alone, even with over-the-counter medications.
Get medical help if withdrawal includes:
Needing help during detox is not a failure or a lack of willpower. Withdrawal places real physical stress on the body, and trying to manage it alone often leads to dehydration, medication side effects, or avoidable complications.
At The Haven Detox, safe drug detox focuses on stabilizing the body safely. Symptoms are monitored around the clock, hydration is supported, and medications are used carefully based on what the body actually needs, not guesswork or trial and error.
If withdrawal feels overwhelming or unsafe, getting professional detox support can protect your health and help you move through this stage more comfortably and safely.
Get answers about your cost / coverage now.
Your information will be kept private
Let’s talk about what’s going on — no judgment. (We’ve been there before ourselves). No one will know you inquired and there is no commitment to call.
Need someone to talk to? We’re always here—day or night.
Ask questions, get guidance—no pressure, no obligation.
Your story stays with us. Confidential support, always.


Why Wait?
Get Answers Now
You’re here because you know you need help. Let’s talk through it together. There’s no commitment and it’s 100% confidential even to check your insurance.
100% Confidential


Why Wait?
Get Answers Now
You’re here because you know you need help. Let’s talk through it together. There’s no commitment and it’s 100% confidential even to check your insurance.
100% Confidential