Get Help Today 24/7

Dr. Rostislav Ignatov, MD
Chief Medical Officer
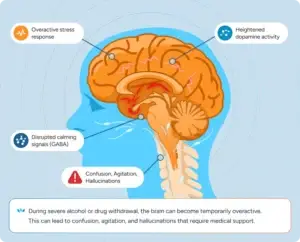
Alcohol withdrawal can push the brain into a state of excessive activity. As the body adjusts to the absence of alcohol, the nervous system can lose its normal braking system, increasing the risk of severe symptoms such as confusion or seizures.
Phenobarbital is considered when withdrawal is putting too much strain on the brain. It is used in specific situations to help stabilize brain activity during higher-risk alcohol detox, not as a routine medication. This page explains when phenobarbital may be used and what families should understand if it becomes part of a detox plan.
Table of Contents
Phenobarbital is used during alcohol detox to reduce dangerous overactivity in the brain when withdrawal is severe. Its primary role is to lower the risk of complications such as seizures and severe confusion.
During alcohol withdrawal, the brain can lose its ability to regulate itself. When that strain becomes difficult to control with standard detox medications, phenobarbital may be used to slow excessive brain activity and help stabilize the nervous system.
In detox, phenobarbital is used short term. It does not treat alcohol use disorder, reduce cravings, or manage long-term symptoms. Its purpose is to protect the brain during the most intense and medically risky phase of withdrawal.
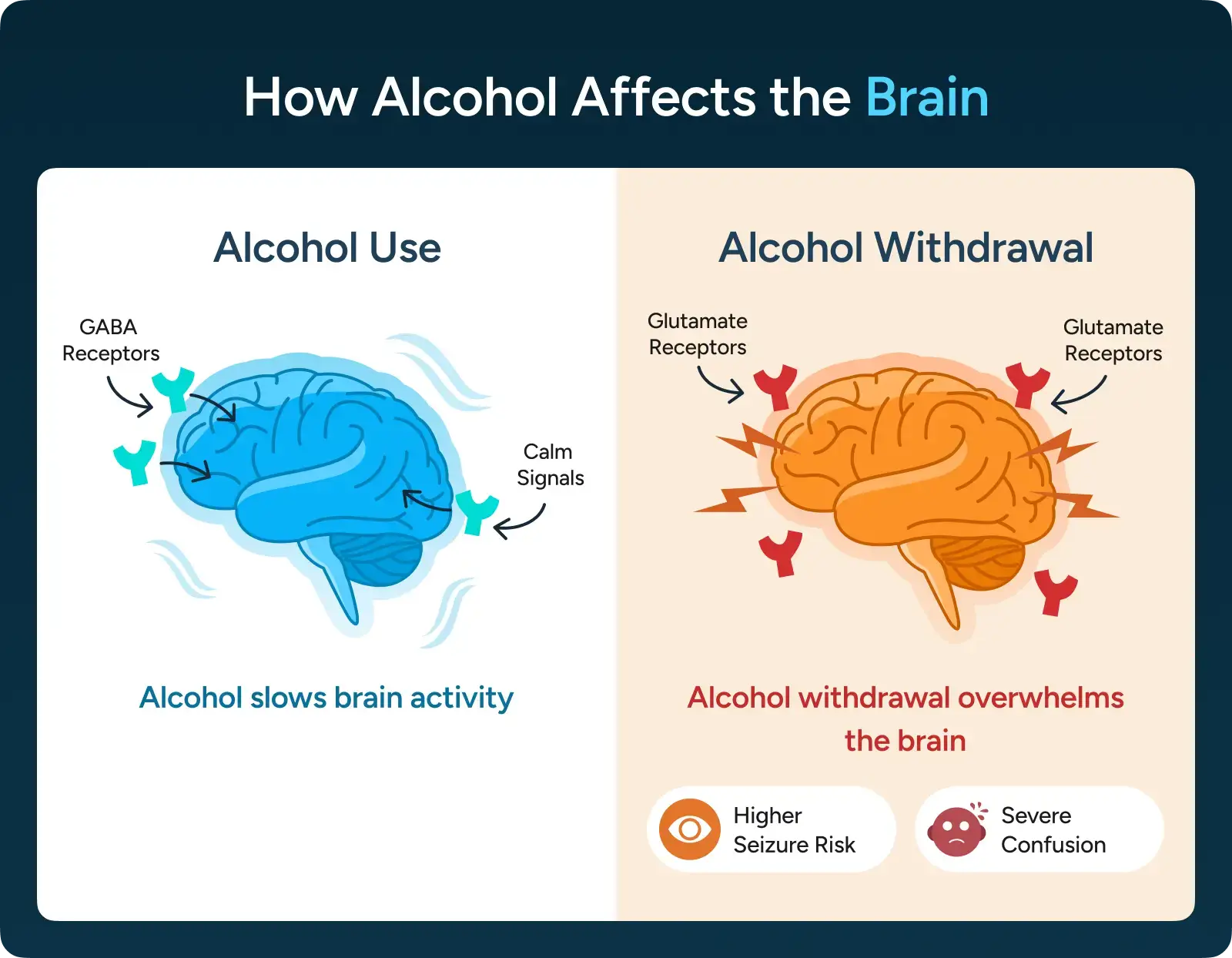
Severe alcohol withdrawal puts the brain into a state of imbalance. Signals that normally slow brain activity become weaker, while signals that increase alertness and excitation become stronger. This shift is what raises the risk of seizures and severe confusion.
Many detox medications rely on the brain’s ability to respond to calming signals. In severe alcohol withdrawal, those calming pathways may not respond as reliably, which can limit how effective some medications are on their own.
Phenobarbital works more broadly. It slows excessive brain activity even when the brain’s normal calming responses are blunted. This allows it to reduce seizure risk and stabilize brain function in situations where withdrawal is placing extreme strain on the nervous system.
This is not about suppressing symptoms completely. It is about preventing the brain from becoming overwhelmed during the most dangerous phase of alcohol withdrawal, while it works to regain balance.
Alcohol changes how the brain keeps itself in balance. Over time, the brain adapts by pushing harder on systems that increase alertness and activity.
When alcohol is removed, those systems do not shut off right away. The brain can become unstable and strained as it tries to recalibrate.
That strain can show up as:
For some people, these symptoms ease with time. For others, the strain increases instead of improving. When withdrawal escalates, it can lead to:
Hospital-based research shows that structured medical care during alcohol withdrawal lowers the risk of serious complications, especially in moderate to severe cases.ⓘ
Phenobarbital is being used more intentionally in severe alcohol withdrawal, particularly when standard detox approaches are not keeping symptoms controlled. This shift is driven by how the medication behaves in the body during high-risk withdrawal, not by nostalgia or changing trends.
Benzodiazepines are effective for many people in mild to moderate alcohol withdrawal. In more severe cases, their effects may wear off quickly, leading to repeated spikes in agitation, confusion, or tremors. This can result in frequent dose adjustments as clinicians try to stay ahead of escalating symptoms.
When withdrawal places sustained strain on the brain, this pattern can make symptom control less predictable.
Phenobarbital stays active in the body much longer than many other detox medications. When used carefully, this longer duration can help keep brain activity steadier during the most dangerous phase of withdrawal, rather than allowing symptoms to surge and crash.
For patients with a history of withdrawal seizures, delirium tremens, or rapidly escalating symptoms, that steadier control can be critical. In these situations, some hospitals and medical detox programs use phenobarbital as part of a protocol-based approach to reduce seizure risk and improve stability.
This does not replace standard detox medications. It reflects a more targeted use of phenobarbital when alcohol withdrawal is severe, unpredictable, or not responding well to first-line treatment.
In some cases, alcohol withdrawal can continue to escalate even with medication. This does not mean something has gone wrong. It means the brain is under extreme stress and needs closer medical support.
When symptoms are not stabilizing, the medical team responds in real time. Doses may be adjusted, additional medications may be used, or care may be escalated to a higher level of monitoring if needed.
This is one of the main reasons alcohol detox should never be attempted at home. If withdrawal becomes more severe, medical teams can act immediately instead of reacting after a crisis has already started.
Phenobarbital is a powerful medication. When it’s used during alcohol detox, dosing has to be precise and the body’s response needs to be watched closely.
As phenobarbital slows brain activity, it can also slow breathing, lower blood pressure, and reduce alertness. Without continuous medical monitoring, those effects can become life-threatening. That’s why phenobarbital is never used at home and is only given in medical detox settings where patients can be watched closely and supported if complications occur.
In medical detox, staff monitor breathing, blood pressure, heart rate, level of sedation, and neurological changes throughout the day and night. If breathing slows, alertness drops, or withdrawal symptoms shift, medications can be adjusted, paused, or stopped immediately.
Phenobarbital also stays in the body longer than many other detox medications. That longer duration can help stabilize severe withdrawal, but it also means dosing decisions have lasting effects and cannot be quickly reversed. This is another reason close medical supervision is required.
Phenobarbital is not intended for long-term use. Its role is short-term protection during the most medically dangerous phase of alcohol withdrawal, when the brain is under the greatest strain.
Phenobarbital is used short term during alcohol detox. It is typically given only during the most intense phase of withdrawal, when medical risk is highest.
For most people, this period lasts a few days, as the brain and nervous system begin to stabilize. As withdrawal symptoms ease, phenobarbital is reduced and discontinued.
Because the medication remains active in the body longer than many other detox medications, it does not need to be given as frequently. This allows for steadier symptom control while the brain adjusts, rather than repeated dosing to chase spikes in agitation or discomfort.
If withdrawal improves as expected, the medication is stepped down. If symptoms persist or shift, dosing may be adjusted briefly to maintain stability.
Phenobarbital affects the brain and nervous system, so some side effects are expected while the medication is active. These effects are monitored closely during medical detox.
Common side effects may include:
These effects are usually temporary and lessen as the dose is reduced and the medication is stopped.
Because phenobarbital can also slow breathing and lower blood pressure, vital signs are monitored throughout detox. If side effects become more pronounced or concerning, the medication can be adjusted or stopped promptly.
In higher-risk alcohol withdrawal, side effects are weighed against risk. Preventing seizures and severe complications takes priority, which is why phenobarbital is used selectively and under medical supervision.
Phenobarbital is not appropriate for every person or every alcohol detox situation. Its use depends on medical history, current health, and how withdrawal is unfolding.
It may be avoided or used with extra caution when there are concerns such as:
Phenobarbital is also not used when alcohol withdrawal is mild and symptoms can be safely managed with less intensive support. In those cases, the risks of a stronger, longer-acting medication may outweigh the benefits.
Phenobarbital is primarily used during alcohol detox. Its main role is to protect the brain when alcohol withdrawal is placing too much strain on the nervous system.
In some cases, phenobarbital may also be used during withdrawal from other sedative medications, such as benzodiazepines or barbiturates, because those substances affect the brain in similar ways to alcohol. These situations are less common and require careful medical oversight.
Phenobarbital is not a standard medication for opioid detox. Opioid withdrawal is extremely uncomfortable, but it does not typically cause the same type of dangerous brain overactivity or seizure risk seen with alcohol or sedative withdrawal. Different medications are used to manage opioid withdrawal safely.
When phenobarbital is included in a detox plan, it is chosen based on the type of substance involved and how withdrawal is affecting the brain—not as a general-purpose detox medication.
Several medications can be used during alcohol detox. Which ones are chosen depends on how much strain withdrawal is putting on the brain and how symptoms are changing over time.
Benzodiazepines are commonly used in alcohol detox, especially in mild to moderate cases. They help calm the nervous system and are effective for many people. In some situations, though, their effects can wear off quickly, leading to repeated symptom spikes that require frequent dosing adjustments.
Phenobarbital works differently. It stays in the body longer and provides more consistent control over brain activity during severe withdrawal. This can help prevent the sharp ups and downs that sometimes occur when symptoms escalate rapidly.
Phenobarbital is more likely to be considered when:
This does not mean phenobarbital is “stronger” or better for everyone. It means it is better suited to certain situations, particularly when withdrawal is placing sustained strain on the brain and requires close medical control. The choice of medication is based on how the body is responding in real time, not on a one-size-fits-all approach.
No. Phenobarbital and benzodiazepines are different types of medications, even though both are sometimes used during alcohol detox.
Benzodiazepines are commonly used first and work by helping the brain respond to calming signals. Phenobarbital works more broadly and stays active in the body longer, which is why it may be used in more severe or high-risk withdrawal situations.
They are not interchangeable, and they are used for different reasons depending on how withdrawal is progressing.
Alcohol withdrawal can change quickly. What starts as shakiness or anxiety can escalate into a medical emergency if the brain is under too much strain.
Medical help should be sought immediately if any of the following are present:
It’s also important to seek help before withdrawal begins if stopping alcohol feels difficult or unsafe. This includes situations where:
Waiting for symptoms to “pass” can be dangerous. Alcohol withdrawal is one of the few types of withdrawal that can be life-threatening, especially with long-term or heavy alcohol use.
Medical detox allows alcohol use to be stopped safely, before withdrawal reaches a crisis point. If there’s uncertainty about how severe symptoms might become, it’s safer to seek help early rather than try to manage it alone.
Get answers about your cost / coverage now.
Your information will be kept private
Let’s talk about what’s going on — no judgment. (We’ve been there before ourselves). No one will know you inquired and there is no commitment to call.
Need someone to talk to? We’re always here—day or night.
Ask questions, get guidance—no pressure, no obligation.
Your story stays with us. Confidential support, always.


Why Wait?
Get Answers Now
You’re here because you know you need help. Let’s talk through it together. There’s no commitment and it’s 100% confidential even to check your insurance.
100% Confidential


Why Wait?
Get Answers Now
You’re here because you know you need help. Let’s talk through it together. There’s no commitment and it’s 100% confidential even to check your insurance.
100% Confidential