
Opioid withdrawal affects more than mood and cravings. It places real stress on the body, including the digestive system. Severe diarrhea, cramping, and fluid loss are common as the body readjusts after opioids are stopped, and for some people, these symptoms become difficult to manage without support in medically supervised detox.
Loperamide, commonly known by the brand name Imodium®, is an over-the-counter medication used to slow intestinal movement and control diarrhea. In medical detox settings, loperamide may be used short-term to help manage severe gastrointestinal symptoms during opioid withdrawal, alongside hydration, monitoring, and other withdrawal medications.
Its role is specific. Loperamide helps control diarrhea and reduce fluid loss, but it does not ease cravings, anxiety, restlessness, or the nervous system changes that drive substance use withdrawal. Because of this, it is used as part of a broader detox plan rather than as a standalone solution.
Knowing how loperamide fits into opioid detox — and where its limits are — can help people make safer decisions during withdrawal and understand why treatment for opioid use disorder often requires medical supervision.
Table of Contents
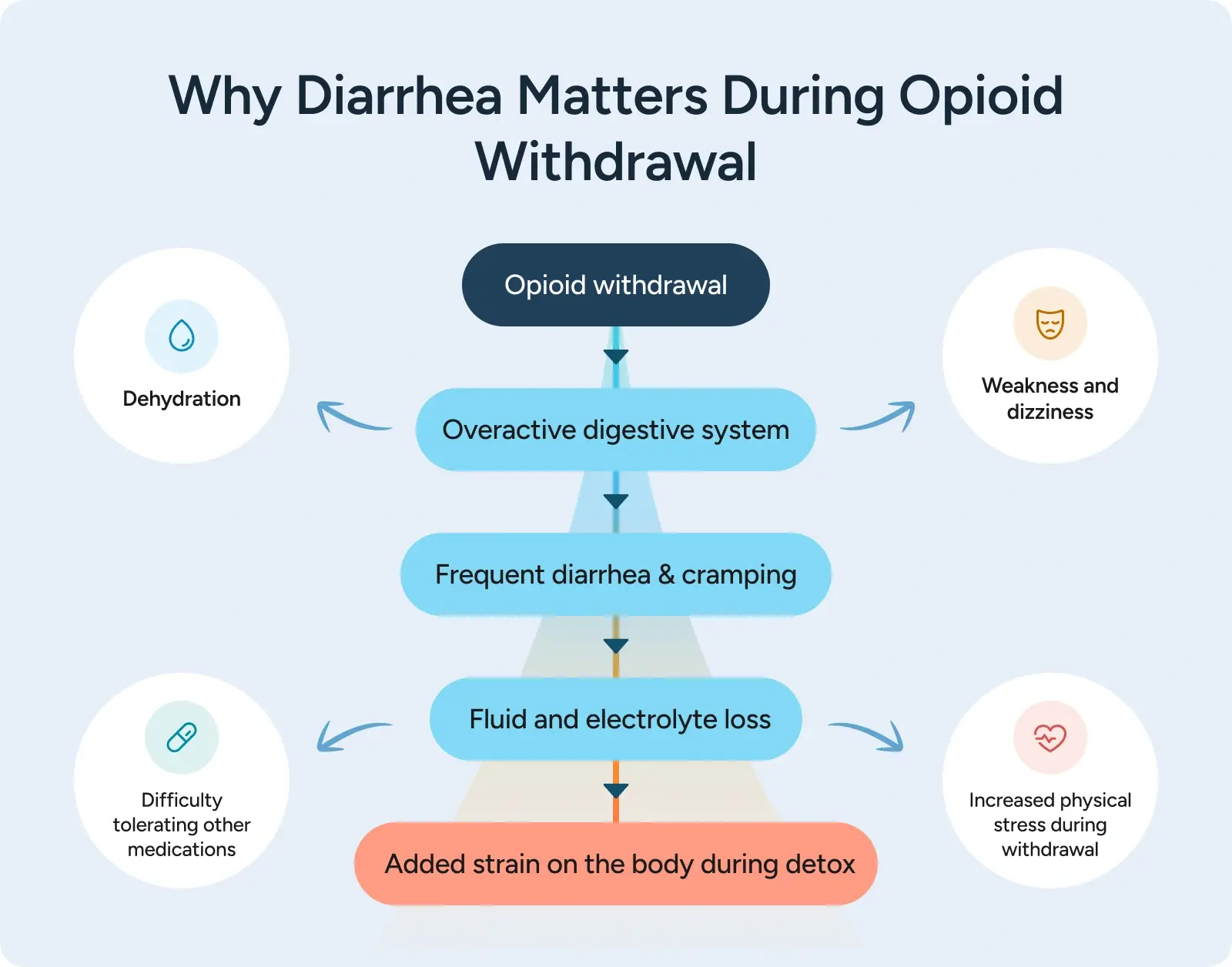
When opioids are stopped, the digestive system often swings in the opposite direction. The intestines become overactive, leading to frequent diarrhea, cramping, and abdominal discomfort.
During withdrawal, this goes beyond inconvenience. Ongoing diarrhea can lead to dehydration and electrolyte loss, which adds strain to the body while the nervous system is already under stress. Fluid imbalance can worsen weakness, dizziness, and fatigue, and it can interfere with the body’s ability to tolerate other withdrawal medications.
For many people, gastrointestinal symptoms become one of the main obstacles to staying stable during medically supervised drug detox.
In medical detox settings, loperamide may be used short-term to control severe diarrhea when fluid loss or repeated bowel movements begin to interfere with hydration and stabilization.
It is given at standard therapeutic doses and used selectively, alongside fluid replacement and monitoring. Loperamide does not treat the broader withdrawal process and is not intended to manage symptoms like cravings, anxiety, or restlessness.
Because it is available over the counter, loperamide is sometimes assumed to be harmless during withdrawal. In detox, its use is deliberate, limited, and focused only on gastrointestinal support within a larger treatment plan.
Loperamide addresses a narrow set of symptoms. While it can help control diarrhea, it does not treat the underlying withdrawal process or the nervous system changes caused by stopping opioids.
Loperamide does not reduce opioid cravings, calm anxiety, ease restlessness, or improve sleep. It does not stabilize heart rate, blood pressure, or temperature changes that often occur during withdrawal. Because of this, it cannot prevent withdrawal from progressing or make detox comfortable on its own.
During medical detox, these symptoms are managed with other medications and clinical support aimed at calming the body’s stress response. Loperamide’s role remains limited to gastrointestinal symptom relief, which is why it is used only as one small part of a broader withdrawal management plan.
When used at standard doses and under medical supervision, loperamide is generally well tolerated. Problems arise when dosing goes beyond recommended limits or when the medication is used without monitoring during withdrawal.
High doses of loperamide can affect the heart’s electrical rhythm, increasing the risk of dangerous arrhythmias. This risk is higher during opioid withdrawal because dehydration and electrolyte imbalances can already place stress on the heart. Symptoms such as palpitations, dizziness, fainting, or unexplained chest discomfort require immediate medical attention.
In medical detox settings, loperamide use is carefully limited and paired with hydration, electrolyte management, and vital sign monitoring. This oversight reduces risk and helps ensure gastrointestinal symptoms are treated without introducing new medical complications.
Because it is available over the counter, loperamide is sometimes assumed to be harmless during withdrawal. In detox, its use is deliberate, limited, and focused only on gastrointestinal support within a larger substance abuse treatment program.
The liver plays a major role in detoxifying both substances and medications. After heavy alcohol use, the liver is often inflamed or damaged, even if blood tests were normal in the past.
Acetaminophen is broken down in the liver. During withdrawal, especially alcohol withdrawal, repeated or higher doses can overwhelm the liver and increase the risk of injury.
At standard doses, loperamide is generally tolerated, but side effects can still occur, especially during opioid withdrawal when the body is already under stress.
Common side effects may include:
In some cases, slowing the digestive system too much can lead to discomfort or worsening abdominal pain.
Because withdrawal can affect hydration, blood pressure, and heart rate, side effects may feel more noticeable during detox than they would otherwise. This is one reason loperamide use is monitored and kept short term in medical settings.
More serious side effects, such as heart rhythm changes, are rare at normal doses but become a concern when dosing exceeds recommendations or when loperamide is used excessively without medical supervision.
Loperamide misuse is uncommon, but when it occurs, it usually falls into a few clear patterns.
Some people take higher-than-recommended amounts while trying to control severe diarrhea, especially if symptoms persist longer than expected. Others use it during opioid withdrawal after encountering online claims that loperamide can ease withdrawal symptoms beyond diarrhea. These claims are misleading and not supported by medical detox protocols.
Misuse typically involves dosing that goes beyond normal use and occurs without medical guidance or monitoring. This is what separates misuse from the limited, symptom-specific use of loperamide during medical detox.
Although loperamide interacts with opioid receptors in the gut, it does not function like opioid medications used in medical detox. It does not cross into the brain at therapeutic doses and does not relieve the central withdrawal symptoms caused by stopping opioids.
This distinction helps explain why loperamide can reduce diarrhea without easing cravings, anxiety, or restlessness during withdrawal.
Opioid withdrawal is rarely life-threatening on its own, but it can become medically complicated when symptoms are severe or difficult to manage at home. This is especially true when diarrhea leads to ongoing fluid loss or when over-the-counter medications are being used to try to control symptoms.
Medical support should be considered if diarrhea is persistent despite standard doses of loperamide, if fluids cannot be kept down, or if weakness, dizziness, or fainting begin to occur. Heart-related symptoms such as palpitations, chest discomfort, or unexplained shortness of breath should always be evaluated right away.
Repeated attempts to get through withdrawal alone can also be a sign that additional support is needed. Programs offering evidence-based addiction treatment provide symptom-specific care, monitoring, and medications that reduce stress on the body while helping people transition safely into recovery.
Getting help during withdrawal is about keeping the body safe while it goes through a lot of stress.
Get answers about your cost / coverage now.
Your information will be kept private
Let’s talk about what’s going on — no judgment. (We’ve been there before ourselves). No one will know you inquired and there is no commitment to call.
Need someone to talk to? We’re always here—day or night.
Ask questions, get guidance—no pressure, no obligation.
Your story stays with us. Confidential support, always.

Why Wait?
Get Answers Now
You’re here because you know you need help. Let’s talk through it together. There’s no commitment and it’s 100% confidential even to check your insurance.
100% Confidential