Get Help Today 24/7

Antipsychotics like Haldol or Zyprexa are sometimes used short-term during alcohol or drug detox when withdrawal symptoms become severe. This page explains why antipsychotics may be used during medically monitored detox, how they fit into medical care, and what families should know about safety, monitoring, and next steps.
Table of Contents
Hearing the word antipsychotic during drug or alcohol detox can be alarming, especially if your loved one has never had a diagnosed mental health condition. In medical detox, antipsychotics are sometimes used short term to help manage severe withdrawal symptoms that can become dangerous without medical support.
During alcohol or drug withdrawal, the brain can enter a temporary crisis state. When symptoms escalate beyond what standard detox medications can safely control on their own, antipsychotics may be added briefly to help calm the nervous system and reduce immediate risk.
This does not mean someone has a chronic psychiatric illness. It does not mean long-term medication is being started. It means the medical team is focused on safety, stabilization, and preventing complications during acute withdrawal.
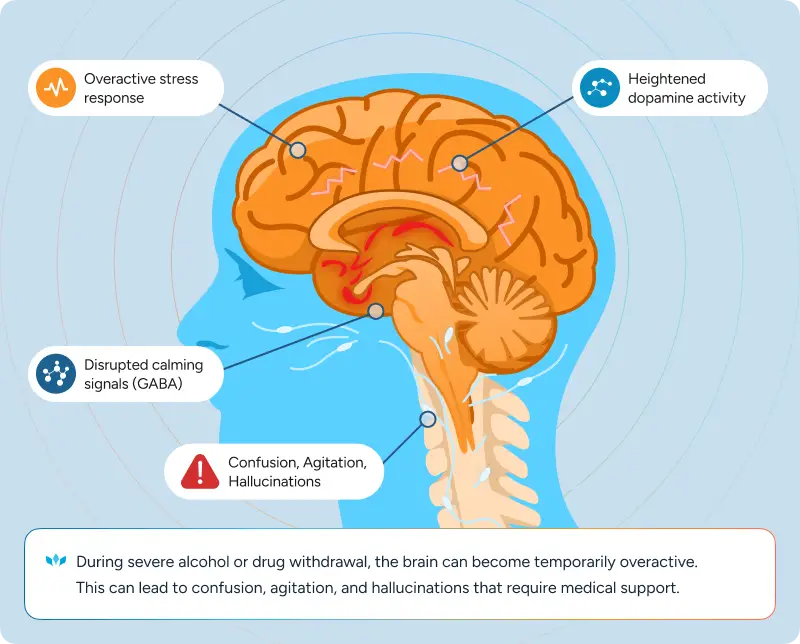
Alcohol and many drugs change how the brain regulates key chemicals like dopamine, glutamate, and GABA (a calming neurotransmitter). When substance use stops suddenly, those systems can rebound aggressively and leave the brain in a hyperactive state.
That overactivity can lead to:
In alcohol detox, these symptoms may be part of delirium tremens (DTs), a serious and potentially life-threatening form of withdrawal. DTs can involve hallucinations, confusion, unstable blood pressure or heart rate, and seizures. This is why medical detox for alcohol withdrawal is critical when symptoms reach this level.
Most medical detox programs rely on proven medications to manage withdrawal safely. Alcohol detox often includes medications to lower seizure risk and calm the nervous system. Opioid detox typically includes medications that reduce withdrawal intensity and help the body stabilize.
In some cases, withdrawal symptoms continue to break through despite appropriate care. Antipsychotics during detox may be considered when:
In these situations, antipsychotics are used as adjunct medical detox medications, not replacements for standard withdrawal treatment. The goal is practical and short term: reduce agitation, improve safety, and allow the rest of the detox plan to work.
One of the biggest fears families have when they hear about antipsychotics in alcohol and drug detox is,
“Are they putting my loved one on a psychiatric medication forever?”
In medical detox, that is not what is happening.
When antipsychotics are used during detox, they are prescribed short-term to manage acute withdrawal symptoms, not to treat a long-term mental health condition. The focus is stabilization, not diagnosis.
Antipsychotics used during detox are typically:
As the brain begins to rebalance after alcohol or drug use stops, the need for these medications often fades quickly. Many patients do not continue antipsychotics beyond the detox phase.
This is a key difference between short-term antipsychotic use in detox and ongoing psychiatric care.
Severe withdrawal can temporarily mimic symptoms of serious mental health conditions. Anxiety, paranoia, mood swings, hallucinations, and confusion can all occur without an underlying psychiatric disorder.
Making long-term diagnoses during this period can be misleading. That is why responsible medical detox programs focus on:
In many cases, symptoms that looked severe during withdrawal improve significantly once detox is complete and the person begins ongoing addiction treatment.
Once withdrawal symptoms settle:
This approach protects patients from unnecessary long-term medications while still addressing severe withdrawal symptoms safely when they occur.
Haldol, also known by its generic name haloperidol, is one of the most commonly used antipsychotics in hospital and emergency settings. In medical detox, it may be used short term to help control severe withdrawal symptoms that put someone at risk.
Its role during detox is specific and limited. Haldol is used short-term to manage severe withdrawal symptoms, not as an ongoing treatment.
Haldol may be considered during alcohol or drug detox when withdrawal symptoms become severe and difficult to manage with standard medications alone.
Common situations include:
In these cases, the goal is rapid stabilization. Calming extreme symptoms early can help prevent medical emergencies and allow the rest of the detox plan to work.
This distinction is important. Haldol in detox is used as an adjunct medication, added only when needed for short-term symptom control.
Because Haldol can affect movement and muscle tone, patients are closely monitored while receiving it during detox.
Possible short-term side effects include:
In a medical detox setting, these effects are watched closely. Doses are adjusted or the medication is stopped if side effects appear or symptoms improve. This level of monitoring is one reason detoxing without medical supervision can be risky when severe symptoms are present.
Haldol vs Zyprexa in Detox
Haldol
Zyprexa
Common use in detox
Speed of effect
Movement side effects
Typical duration
Severe agitation, delirium
Faster
More common
Short term
Agitation, anxiety, sleep
More gradual
Less common
Short term
Haldol
Common use in detox
Severe agitation, delirium
Speed of effect
Faster
Movement side effects
More common
Typical duration
Short term
Zyprexa
Common use in detox
Agitation, anxiety, sleep
Speed of effect
More gradual
Movement side effects
Less common
Typical duration
Short term
Zyprexa, also known as olanzapine, is a newer antipsychotic that may be used during drug or alcohol detox when symptoms are intense but constant heavy sedation is not the goal. Like Haldol, it is used short term and reassessed as symptoms change.
Zyprexa is often chosen when the treatment team needs symptom control that feels steadier and more tolerable as the nervous system calms.
Zyprexa may be considered when withdrawal symptoms include:
For some patients, Zyprexa can help take the edge off intense symptoms without the same movement-related side effects seen more commonly with older antipsychotics.
Zyprexa belongs to a newer group of antipsychotics sometimes called “atypical” antipsychotics. In the context of detox, that difference matters.
Compared to older medications like Haldol:
These qualities can make Zyprexa a better short-term option for patients whose symptoms are severe but not immediately dangerous.
When used during medical detox, Zyprexa is:
Possible short-term side effects may include:
In a medical detox setting, staff monitor for these effects and adjust care as needed. The goal is always symptom relief with the least medication necessary, for the shortest amount of time possible.
Antipsychotics are not part of every detox plan. They are used selectively and only when symptoms become severe enough to raise safety concerns. In medical detox, these medications support stabilization. They do not replace the primary treatments used for alcohol or drug withdrawal.
Medical detox is built around medications that directly treat withdrawal.
Depending on the substance involved, this may include:
Antipsychotics during detox may be added when symptoms such as hallucinations, paranoia, or severe agitation persist despite appropriate use of these medications. In this role, antipsychotics act as adjunct medical detox medications, not replacements.
The decision to use antipsychotics during drug or alcohol detox is based on real-time medical assessment.
Factors include:
Because withdrawal symptoms can change quickly, medication plans are reassessed daily and adjusted as the nervous system begins to stabilize.
Severe withdrawal is unpredictable, especially during alcohol detox. Medical detox allows medications to be adjusted quickly, symptoms to be treated early, and complications to be prevented.
This level of care is especially important when confusion, paranoia, or hallucinations are present, and it is one of the key reasons medical detox is safer than attempting withdrawal alone.
Any medication used during detox needs careful oversight, especially when symptoms are severe. This is true for antipsychotics, as well as for standard detox medications. Safety comes from close monitoring, frequent reassessment, and short-term use, not from the medication alone.
In a medical detox setting, patients are monitored around the clock. This allows staff to track how the body is responding to both withdrawal and medication support.
Monitoring typically includes:
Because withdrawal symptoms can shift quickly, this ongoing observation is critical when antipsychotics are part of the detox plan.
When antipsychotics like Haldol or Zyprexa are used short-term during detox, side effects are usually temporary and dose-related.
Depending on the medication, these may include:
These effects are watched closely. If side effects appear or symptoms improve, doses can be reduced or the medication can be stopped altogether.
Trying to manage withdrawal at home can feel like the easiest or least disruptive option, especially early on. But when symptoms move beyond mild discomfort, at-home detox becomes unpredictable and, in some cases, dangerous.
Severe withdrawal can include:
These symptoms can escalate quickly, particularly during alcohol withdrawal, and what feels manageable early can become a medical emergency within hours.
At home, there is no way to:
Another concern is medication misuse. Taking leftover prescriptions, borrowing medications, or combining substances to “take the edge off” can unintentionally worsen confusion, slow breathing, or increase the risk of dangerous interactions.
Medical detox provides a controlled environment where:
When hallucinations, paranoia, or severe agitation appear, detoxing alone is no longer just uncomfortable. It becomes unsafe.
In many cases, yes. When severe withdrawal symptoms are treated early and appropriately, the risk of serious medical complications drops significantly.
Uncontrolled withdrawal puts extreme stress on the brain and body. Hallucinations, confusion, and severe agitation are not just distressing. They can lead to falls, injuries, dehydration, heart rhythm problems, seizures, and emergency hospitalizations.
Short-term use of medications, including antipsychotics during detox, can help interrupt that escalation.
When used carefully in a professional medical detox setting, these medications may:
This kind of early intervention can also reduce emotional trauma. Severe, unmanaged withdrawal can be frightening and disorienting, and those memories can linger long after detox is over. Calming symptoms safely can make the experience more tolerable and protect long-term mental health.
Just as important, stabilization during detox creates a clearer starting point for ongoing treatment. Once the nervous system settles, care decisions can be made thoughtfully rather than reactively.
Withdrawal does not always look dramatic at first. Symptoms can build quietly, then escalate faster than expected. Knowing when to reach out for medical detox can prevent emergencies and reduce unnecessary suffering.
Medical detox should be considered right away if alcohol or drug withdrawal includes:
These are signs that the nervous system is under significant stress and needs medical support.
Medical detox provides a safer alternative to trying to push through withdrawal alone. Care includes:
If you are unsure whether symptoms are serious enough, calling early can help prevent a dangerous situation.
Reaching out for help is not about overreacting. It is about protecting yourself or loved one and giving withdrawal the support it sometimes requires.
Get answers about your cost / coverage now.
Your information will be kept private
Let’s talk about what’s going on — no judgment. (We’ve been there before ourselves). No one will know you inquired and there is no commitment to call.
Need someone to talk to? We’re always here—day or night.
Ask questions, get guidance—no pressure, no obligation.
Your story stays with us. Confidential support, always.


Why Wait?
Get Answers Now
You’re here because you know you need help. Let’s talk through it together. There’s no commitment and it’s 100% confidential even to check your insurance.
100% Confidential


Why Wait?
Get Answers Now
You’re here because you know you need help. Let’s talk through it together. There’s no commitment and it’s 100% confidential even to check your insurance.
100% Confidential